If you are looking for information on osteoporosis treatment, you are not alone. Over 1.2 million Australians are currently living with osteoporosis and an additional 5 million have osteopenia or poor bone health — and that figure does not capture the many more who remain undiagnosed. Osteoporosis treatment in Australia today encompasses a wide spectrum of options: from prescription medications and calcium supplementation through to targeted osteoporosis exercise programs and osteogenic loading. Understanding what works, what doesn’t, and what is right for your individual circumstances is the first step.
At OsteoStrong® Australia, our mission is to help people live their best lives, for longer — and that starts with the foundation of the body: your skeleton. This guide walks you through the full landscape of osteoporosis treatment options available in Australia, including the science on which types of exercise actually build bone density, so you can make informed decisions alongside your healthcare team.
This information is general in nature and is not intended as medical advice. Always consult your GP or a qualified healthcare professional for personalised guidance regarding osteoporosis treatment and management.
What Is Osteoporosis? Understanding the Condition
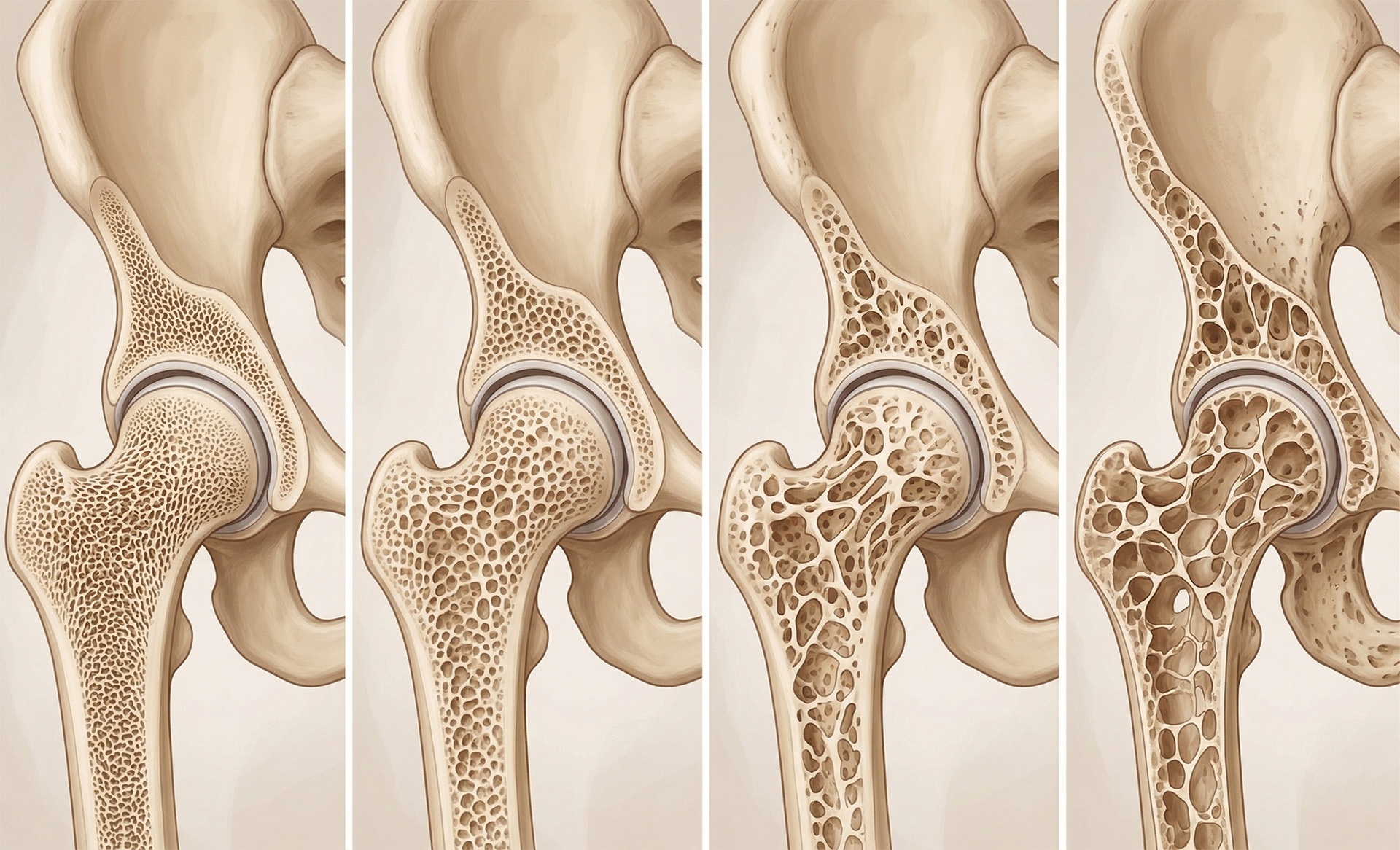
Osteoporosis is a condition in which bones progressively lose density and structural strength, making them fragile and significantly more susceptible to fractures — sometimes from a minor fall, or even normal daily movements. Often called the ‘silent disease’, it typically develops without any symptoms until a fracture occurs.
Bone density peaks in your late twenties, then begins to slowly decline from around age 35. In women, this decline accelerates significantly after menopause due to the drop in oestrogen, a hormone that plays a key role in maintaining bone mass. However, osteoporosis is far from exclusively a women’s health issue: 65% of Australian men over 70 have been diagnosed with either osteopenia or osteoporosis, and 1 in 3 men will experience an osteoporotic fracture in their lifetime.
How Is Osteoporosis Diagnosed?
The standard diagnostic tool for osteoporosis in Australia is a DEXA scan (dual-energy X-ray absorptiometry), which measures bone mineral density (BMD). Results are given as a T-score:
| DEXA T-SCORE | BONE HEALTH |
| 0 | Benchmark based on a Healthy 30 year old bone density |
| -1.0 or above | Normal Bone Density |
| -1.0 to -2.5 | Osteopenia (low bone density, a precursor to osteoporosis) |
| -2.5 or less | Osteoporosis |
Your GP may also use a fracture risk assessment tool such as FRAX, which takes a range of clinical factors into account to estimate your 10-year probability of a fracture — helping guide decisions about when osteoporosis treatment is appropriate.
Osteoporosis Treatment Options in Australia
Effective osteoporosis treatment in Australia is rarely a single intervention. It typically involves a personalised combination of approaches based on your DEXA results, fracture risk, age, and overall health. Below is a comprehensive overview.
1. Prescription Medication for Osteoporosis
Medication is often a central component of osteoporosis treatment for people with a confirmed diagnosis or high fracture risk. All medications should be discussed with and prescribed by your GP or specialist.
- Bisphosphonates (alendronate, risedronate, zoledronic acid) — the most commonly prescribed osteoporosis medications in Australia. They slow the breakdown of bone and can have long-lasting effects. Duration of treatment is typically reviewed after 3–5 years.
- Denosumab — a biologic injection given every six months, now the most widely used osteoporosis medication in Australia. It works by blocking a protein that triggers bone resorption. Bone density can decline if treatment is stopped, so cessation must be carefully managed to prevent rebound vertebral fracture.
- Hormone replacement therapy (HRT) — for post-menopausal women, HRT can help preserve bone density. Suitability is assessed individually based on overall health profile.
- Osteoanabolic therapies (teriparatide, romosozumab) — newer agents that actively stimulate bone formation rather than simply slowing breakdown. Typically prescribed by specialists for severe or high-risk cases. The updated 2024 RACGP/Healthy Bones Australia guidelines emphasise the importance of earlier use of these osteoanabolic therapies for those at ‘imminent’ or ‘very high’ fracture risk.
All osteoporosis medications carry potential side effects and important considerations and are most effective when combined with appropriate lifestyle measures. Treatment decisions should always be made in partnership with your healthcare team.
2. Calcium and Vitamin D
Calcium and vitamin D are foundational to bone health and form an important part of any osteoporosis treatment plan — though the 2024 RACGP guidelines note that supplementation is most effective in people who are actually deficient, and should not be seen as a stand-alone first-line treatment.
- Recommended daily calcium intake for Australians over 50: 1,300 mg per day.
- Vitamin D is essential for calcium absorption from the gut. Deficiency is common in Australia, particularly in southern states and among people who spend limited time outdoors.
- Dietary sources are preferable where possible; supplementation should be guided by your GP based on blood test results. No studies show evidence of improvement in BMD using these supplements in isolation.
3. Osteoporosis Exercise: What the Evidence Actually Says
Exercise is one of the most important non-pharmacological components of osteoporosis treatment — but not all types of exercise are equally effective at building bone density. This is one of the most misunderstood areas of bone health, and it is important to get it right.
What the evidence says about low-impact exercise and walking
Walking is widely recommended for general health — and it is a valuable form of physical activity. However, the scientific evidence is clear: low-impact and non-weight-bearing exercise such as walking, swimming, Tai Chi, Pilates, yoga, and cycling have little to no ability to improve bone mass in older adults.
Multiple meta-analyses have confirmed that walking alone produces no significant effect on bone mineral density at the lumbar spine or femoral neck — the two sites most vulnerable in osteoporosis. Healthy Bones Australia’s Exercise Prescription Guidelines (2024) state explicitly that “non-weightbearing and low-impact exercise … have little to no ability to improve bone mass in older age” and “do not comprise a therapeutic recommendation for the purpose of increasing bone mass or even preventing bone loss.”
This does not mean walking has no value — it supports cardiovascular health, mental wellbeing, and may assist with fall prevention through general conditioning. But if your goal is to increase bone density as part of your osteoporosis treatment, walking alone will not achieve it.
The types of osteoporosis exercise that do build bone density
Bone adapts to load. The greater the force applied to the skeletal system — safely, progressively, and with appropriate frequency — the stronger the osteogenic (bone-building) response. This challenges conventional advice that more exercise is always better. When it comes to bone health, it’s the magnitude of load, not the frequency, that drives results.
This principle, known as Wolff’s Law, is the scientific foundation upon which OsteoStrong® was built.
The exercise approaches with the strongest evidence for improving bone mineral density are:
- High-load, progressive resistance training — using free weights or machine-based resistance at moderate-to-high loads (generally 8 or fewer repetitions per set). Resistance training at sufficient intensity has demonstrated consistent improvements in bone density, particularly at the lumbar spine, and is recommended as a core component of osteoporosis exercise by Healthy Bones Australia.
- High-impact weight-bearing activity — such as jumping, hopping, and landing. These activities generate high strain rates through the skeletal system and can be osteogenic, but must be prescribed carefully and are generally contraindicated in people with severe osteoporosis or recent fractures due to fracture risk.
- Osteogenic loading — a specialised, science-based method that applies a precise, safe, and measurable level of force to the skeletal system to trigger bone remodelling. Unlike conventional resistance training or high-impact exercise, osteogenic loading achieves the necessary bone-building stimulus in a controlled, slow, and highly safe manner — making it suitable for people of almost any age or fitness level, including those with established osteoporosis and previous fractures (subject to medical clearance for moderate weight bearing exercise).
The OsteoStrong® difference: The Spectrum® osteogenic loading system used at OsteoStrong® centres is specifically designed to apply the precise level of skeletal force required to trigger the body’s natural bone-building process — safely, without heavy weights, high impact, or sweating. Sessions take less than 15 minutes, once per week. It is the only technology of its kind available in Australia.
More than 14 million osteogenic loading sessions have been delivered globally in OsteoStrong® Centres in over 15 Countries over the past decade.
What other forms of exercise contribute to osteoporosis management
While low-impact activities may not directly build bone density, they do play a valuable supporting role in osteoporosis management:
- Balance, strength, and stability training — Tai Chi, single-leg exercises, and targeted balance work reduce fall risk, which is critically important for people with osteoporosis. Research confirms that well-designed balance and strength programs can reduce the rate of falls resulting in fractures by more than 60%.
- Postural training — exercises that strengthen the muscles supporting the spine and improve posture help reduce the risk of vertebral fractures and the characteristic ‘stooping’ associated with spinal osteoporosis.
- Flexibility and mobility — gentle stretching and mobility work support functional movement and quality of life, though forward spinal flexion should be avoided in people with vertebral osteoporosis.
Important: always seek guidance from your healthcare team before beginning any new exercise program. High-impact activities and exercises involving forward bending at the spine or impacts can increase fracture risk in people with established osteoporosis.
4. Fall Prevention
Preventing falls is as critical as building bone strength in osteoporosis treatment. A fall that causes a bruise in someone with healthy bones can cause a life-altering fracture — particularly at the hip, wrist, or spine — in someone with low bone density. Hip fractures in particular carry serious consequences: mortality in the first year after a major osteoporotic fracture can be up to three times higher than in age-matched individuals.
Practical fall prevention strategies include:
- Supervised balance and strength training as part of your osteoporosis exercise program
- Reviewing your medications with your GP (some medications increase dizziness or fall risk)
- Regular vision and hearing checks
- Home safety modifications — removing trip hazards, improving lighting, installing grab rails
- Wearing supportive, well-fitting footwear
5. Nutrition for Bone Health Beyond Calcium
Optimal bone health requires more than calcium alone. A well-balanced, anti-inflammatory diet supports the entire musculoskeletal system and complements your overall osteoporosis treatment plan.
- Protein — essential for both bone matrix formation and muscle maintenance. Due to age-related declines in digestion and protein synthesis, emerging evidence suggests adults over 50 consume 1.2–1.6 grams per kg body weight per day (current U.S. FDA guidance), with intakes up to 2.0 g/kg/day potentially appropriate for older or osteoporotic individuals—subject to individual clinical considerations.
- Vitamin K2, vitamin C, magnesium, boron, Iodine, and zinc — support bone metabolism, thyroid health, and how the body uses calcium effectively.
- Minimise bone-depleting habits — smoking, excessive alcohol, very high caffeine, and, soda drinks, and high sodium intake can all negatively impact bone health over time.
How OsteoStrong® Supports Your Osteoporosis Treatment
OsteoStrong® is a natural, non-invasive program designed to complement your osteoporosis treatment by harnessing the body’s own ability to build stronger bones — without medication, heavy weights, or high-impact exercise.
The patented Spectrum® osteogenic loading system — available exclusively at OsteoStrong® centres — applies a safe, controlled, and precisely measured force to the skeletal system during each weekly session. This is specifically designed to trigger osteogenesis: the biological process by which your body lays down new bone tissue.
Because bone adapts to the magnitude of load—higher forces drive greater adaptation. An important point of difference between most other exercise, is that at OsteoStrong®, you’re positioned in your strongest biomechanical range, allowing 8–10× greater force production. This enables a powerful osteogenic stimulus with just one repetition on each of four machines—no exhaustive, repetitive workouts required.
A typical OsteoStrong® session takes less than 15 minutes, just once a week. You don’t need to be fit to start. Every session is individually supervised and tailored to your needs, health history, and goals. Progress is tracked through regular baseline testing so you and your healthcare team can monitor results over time.
The OsteoStrong® program meets and exceeds the RACGP guidelines for osteoporosis prevention, diagnosis and management. No GP referral is required, though we actively welcome referrals and share-care arrangements with GPs, endocrinologists, rheumatologists, and allied health professionals.
“After a low-impact fracture in July 2023, my DEXA scan revealed Osteoporosis. A 12-month follow-up DEXA scan showed I had improved my lumbar spine T-score from -3.0 to -2.6. I’m converted for sure and never miss a week!”
Jodie, OsteoStrong® Ballarat Member
Frequently Asked Questions About Osteoporosis Treatment
What is the most effective treatment for osteoporosis in Australia?
Effective osteoporosis treatment in Australia is generally a combination of approaches: prescription medication where clinically indicated, adequate calcium and vitamin D, targeted osteoporosis exercise (specifically high-load resistance training or osteogenic loading), fall prevention, and dietary support. The right combination depends on your individual DEXA results, fracture risk score, age, and overall health. Your GP or specialist will guide you through the appropriate options.
Does walking help osteoporosis?
Walking has many benefits for general health and wellbeing, but the scientific evidence shows it has little to no effect on improving bone mineral density in older adults. Multiple meta-analyses confirm that walking alone produces no significant improvement at the lumbar spine or femoral neck — the sites most vulnerable to osteoporotic fractures. For bone density improvement, higher-load resistance training or osteogenic loading is required. Walking can, however, support general conditioning and fall prevention as part of a broader osteoporosis management plan.
What is the best exercise for osteoporosis?
The best osteoporosis exercise for building bone density is moderate-to-high load resistance training or osteogenic loading — both of which apply sufficient mechanical force to the skeleton to trigger the bone-building process (osteogenesis). Balance training and postural exercises are also important for reducing fall and fracture risk. Low-impact activities such as walking, swimming, and yoga support general health but do not directly improve bone mineral density. Always consult your healthcare team before starting a new exercise program.
Can osteoporosis be reversed naturally?
Osteoporosis cannot always be fully reversed, but meaningful improvements in bone mineral density are achievable with the right treatment approach. Hundreds of Australian OsteoStrong® members have reported that they have achieved measurable improvements in their DEXA scan results through weekly osteogenic loading sessions. Individual results vary, and bone density changes are best tracked through DEXA scans conducted every one to two years. Always work with your healthcare team to set realistic, evidence-based goals for your bone health.
Do I need a GP referral for OsteoStrong®?
No GP referral is required to begin the OsteoStrong® program. However, we may request medical clearance for members with certain pre-existing conditions or recent fractures. We also welcome and actively encourage referrals from GPs and allied health professional and can provide relevant progress reports to your treating team on request.
Working With Your Healthcare Team
OsteoStrong® is not a replacement for medical care — it is a powerful, evidence-based complement to it. We encourage all members to continue working closely with their GP, endocrinologist, rheumatologist, physiotherapist, chiropractor or other relevant specialists. A collaborative, whole-person approach to osteoporosis treatment will always produce the best outcomes.
We are happy to share relevant progress reports with your healthcare providers and specialists on request, and warmly welcome enquiries from medical and allied health professionals seeking evidence-based, natural options to support their patients.
Take the First Step Towards Stronger Bones
Whether you have just received a diagnosis, have been managing osteoporosis for some time, or simply want to get ahead of the ageing process — it is never too late to take proactive steps. OsteoStrong® has supported members in their 50s, 60s, 70s, 80s, and 90s to make measurable progress towards stronger bones, better balance, and a longer, more independent life.
Book a complimentary Discovery Session
Visit your nearest OsteoStrong® centre and discover how our scientifically grounded, natural approach to bone health can complement your osteoporosis treatment plan.
Find a centre: osteostrong.com.au/locations
IMPORTANT NOTICE
The information in this article is general in nature and provided for educational purposes only. It is not intended as professional or medical advice, and should not be used to diagnose, treat, cure, or prevent any disease or health condition. It is not a substitute for advice from a qualified healthcare professional.
Individual suitability for the OsteoStrong® program is determined through pre-activity screening. Medical clearance may be required for certain pre-existing conditions prior to commencing physical activity.
Always consult your GP or qualified healthcare professional before making decisions about osteoporosis treatment or commencing any new exercise program.